Drug information
| drug-audio-en-Vorinostat.mp3 |
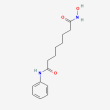
C14 H20 N2 O3
N'-hydroxy-N-phenyloctanediamide
Vorinostat is in Phase 2 development as a latency-reversing agent for HIV.
vorinostat
Molecular Weight: 264.32
(Compound details obtained from PubChem1 and Treatment Action Group website2)
Pharmacology
Mechanism of Action
Latency-reversing agent, specifically a histone deacetylase inhibitor (HDACi).2 Vorinostat, a hydroxamic acid, is a pan-HDACi of class I and II histone deacetylases (HDACs).3 Vorinostat is FDA-approved under the brand name Zolinza for the treatment of cutaneous T-cell lymphoma.4 As an HIV therapeutic, vorinostat is being investigated as an agent for reactivating latent HIV expression.2
In HIV-1 latency, HDACs are recruited to the proviral 5' long terminal repeat (LTR), where they catalyze deacetylation of lysine residues on histones, resulting in chromatin condensation on nucleosome 1 (nuc-1) and preventing HIV transcription. Inhibition of HDAC activity, however, causes histone acetylation (hyperacetylation) of lysine residues by histone acetyltransferases (HATs). This leads to chromatin relaxation and transcriptional activation of HIV.3,5 Some research suggests that the activity of HDACis in inducing HIV transcription may not be caused by direct effects on histone acetylation, but may be caused by effects on other nonhistone proteins.6-8
Half-life (T½)
After oral administration of vorinostat in patients with advanced cancer, the mean terminal half-life of vorinostat was approximately 2 hours, and the mean terminal half-lives of vorinostat’s two inactive metabolites, O-glucuronide and 4-anilino-4-oxobutanoic acid, were approximately 2 hours and 11 hours, respectively.4
Metabolism/Elimination
Vorinostat is eliminated primarily through metabolism via glucuronidation and hydrolysis (major pathways), followed by β-oxidation. CYP enzymes have a negligible role in vorinostat metabolism. Less than 1% of a total vorinostat dose is recovered as unchanged drug in urine, indicating that vorinostat is not excreted renally. At steady state, approximately 16% of a vorinostat dose is excreted in the urine as the inactive metabolite O-glucuronide and approximately 36% is excreted in the urine as the inactive metabolite 4-anilino-4-oxobutanoic acid.4
Select Clinical Trials
Study Identifier: NCT01319383
Sponsor: University of North Carolina, Chapel Hill
Phase: 1/2
Status: This study has been completed.
Study Purpose: The purpose of this open-label study was to determine the efficacy of vorinostat in inducing HIV RNA expression within resting CD4 cells after single and multiple short-interval vorinostat doses.
Study Population:
- Participants were adults with HIV who were receiving stable ART.
- Participants had HIV-1 RNA <50 copies/mL and CD4 cell counts >300 cells/mm3 for at least 6 months before study entry.9,10
Selected Study Results: Results published in Nature (2012), The Journal of Infectious Diseases (2014), and The Journal of Clinical Investigation (2017) showed that both a single dose of vorinostat and paired doses of vorinostat (with each dose separated by 72 hours) was capable of activating latent HIV in a majority of the participants studied. Multiple cycles of daily dosing with vorinostat, however, had only a minimal effect on reactivating HIV latency.10-12
Study Identifiers: (1) SEARCH 019; NCT02475915 and (2) SEARCH 026; NCT02470351
Sponsor: SEARCH Research Foundation
Phase: 1/2
Status: These studies have been completed.
Study Purpose:
- The purpose of the open-label SEARCH 019 trial was to compare the safety and effectiveness of vorinostat plus hydroxychloroquine plus maraviroc (VHM) in combination with ART versus ART alone in controlling HIV RNA during an analytical treatment interruption (ATI) that followed.
- SEARCH 026 was a substudy designed to evaluate the effects of SEARCH 019 study interventions on the central nervous system (CNS).
Study Population:
- Participants were adults with HIV who initiated ART during acute HIV infection.
- Participants had HIV RNA <50 copies/mL for at least 28 weeks prior to enrollment and CD4 counts >450 cells/mm3.13-15
Selected Study Results: Findings from the primary study (SEARCH 019) published in the Journal of Virus Eradication (2020) showed that vorinostat, hydroxychloroquine, and maraviroc added to ART was not more effective in controlling viral load levels during a treatment interruption than ART given alone.15
Additional Published Material:
- AIDS, 2016: Central nervous system impact of vorinostat, hydroxychloroquine and maraviroc combination therapy followed by treatment interruption in individuals treated during acute HIV infection (SEARCH 026)
Study Identifier: NCT01365065
Sponsor: Bayside Health
Phase: 2
Status: This study has been completed.
Study Purpose: The purpose of this open-label study was to determine the ability of vorinostat to induce HIV RNA expression within resting CD4 cells after 14 days of daily vorinostat.
Study Population:
- Participants were adults with HIV who were receiving suppressive ART.
- Participants had HIV-1 RNA <50 copies/mL for at least 3 years and CD4 counts >500 cells/mm3.2,16
Selected Study Results: Results published in PLoS Pathogens (2014) demonstrated that vorinostat given once daily for 14 days was able to significantly activate latent HIV expression in the majority of participants studied.6
Study Identifiers: RIVER trial; NCT02336074
Sponsor: Imperial College London
Phase: 2
Status: This study has been completed.
Study Purpose: The purpose of this open-label, proof-of-concept study was to determine whether a combined approach using ART plus two anti-HIV vaccines and vorinostat could lead to greater reductions in the size of the latent HIV reservoir when compared to ART alone.
Study Population:
- Participants were adults with HIV. Participants who were enrolled in this study had been diagnosed with primary HIV infection within 4 weeks of enrollment.17,18
Selected Study Results: Results published in Lancet (2020) showed that this combination approach of ART, therapeutic HIV vaccines, and vorinostat did not prove to be any more beneficial than ART given alone in reducing latent HIV reservoir size.19
Additional Published Material:
- Sci Rep article, 2023: Therapeutic vaccination following early antiretroviral therapy elicits highly functional T cell responses against conserved HIV-1 regions
Study Identifiers: MOXIE trial; ACTG A5366; NCT03382834
Sponsor: National Institute of Allergy and Infectious Diseases (NIAID)
Phase: 2
Status: This study has been completed.
Study Purpose: The purpose of this open-label trial was to evaluate whether the selective estrogen receptor modulator tamoxifen could enhance vorinostat’s ability to reverse HIV latency in post-menopausal women with HIV who were virologically suppressed on ART.
Study Population:
- Participants were women who were postmenopausal and had HIV.
- Participants had been virologically suppressed for at least 1 year and had been receiving continuous ART for at least 2 years prior to study enrollment.
- Participants had CD4 counts >300 cells/mm3.20,21
Selected Study Results: Findings presented at CROI 2020 and published in Clinical Infectious Diseases (2022) showed that treatment with tamoxifen and vorinostat was not associated with any Grade 3 or higher adverse events (AEs). Tamoxifen did not enhance the magnitude of latent HIV activation with vorinostat in postmenopausal women.21,22
Other early-phase studies investigating vorinostat for HIV treatment have been conducted, including:
- XTRA trial (NCT03212989): A Phase 1 study that evaluated the effects of vorinostat and HIV-1 antigen expanded specific T-cell therapy on persistent HIV in individuals on suppressive ART. This study has been completed, and results are available from IAS 2023 and J Infect Dis (2024).23
- VOR-07 study (NCT03803605): A Phase 1 study that evaluated the effects of vorinostat and the investigational broadly neutralizing antibody VRC07-523LS on persistent HIV in individuals on suppressive ART. This study has been completed, and results are available from IAS 2021 and J Infect Dis (2022).24
- DART DELIVER-02 study (NCT07217379): A Phase 1 study evaluating the safety, tolerability, pharmacokinetics, and immunogenicity of two investigational antibodies for HIV, MGD014 and MGD020, administered alone and in combination with vorinostat or a temporary treatment interruption of ART. This study is currently recruiting participants.25
Adverse Events
NCT01319383
In this Phase 1/2 study, no vorinostat-associated AEs were reported during single limited exposures to vorinostat in eight participants with HIV on suppressive ART. No AEs greater than Grade 1 severity occurred.11 During multiple short-interval vorinostat dosing (every 24 hours) in five participants, some mild, transient gastrointestinal symptoms and headache occurred (all below Grade 1 severity). Transient thrombocytopenia occurred in all participants. Only one participant developed Grade 1 thrombocytopenia, and this toxicity level was observed at just a single study visit.12 A neurocognitive assessment performed on all five participants at baseline and study end found no significant change in neurocognitive functioning.26
During another study conducted under this same protocol evaluating single dosing, paired dosing, and multiple dosing (every 72 hours) of vorinostat, similar AEs were reported. Mild and transient gastrointestinal symptoms (below Grade 1) occurred and transient thrombocytopenia (below Grade 1) was seen in the participants who received multiple vorinostat dosing.10
SEARCH 019 (NCT02475915) and SEARCH 026 (NCT02470351)
In the SEARCH 019 study, serious adverse events (SAEs) occurred in two out of 10 participants in the VHM arm. One of the two participants discontinued the study because of renal insufficiency plus low platelets (VHM-related), and the other participant had diarrhea (possibly due to food poisoning/VHM). In terms of nonserious AEs, 81 events occurred in 10 ART plus VHM participants, and 37 events occurred in five ART-only participants. Significantly more participants in the ART plus VHM group than in the ART-only group experienced nonserious thrombocytopenia and elevated creatinine levels. There were no reports of acute retroviral syndrome following ATI. Additionally, following ATI, there were no new resistance mutations detected and no reports of virological failure after participants resumed ART.13,27
The CNS substudy found that VHM treatment did not result in detectable CSF HIV RNA or in lasting adverse effects—this was based on CSF inflammatory measures, neuropsychological testing, and magnetic resonance spectroscopy (MRS). ATI was found to be associated with CNS immune activation and detectable HIV RNA in CSF.14,28
NCT01365065
In this Phase 2 study, 90% (18/20) of study participants experienced a Grade 1 or 2 AE, with nausea, diarrhea, fatigue, and thrombocytopenia being the most common AEs. There was no occurrence of AEs of a higher grade, dose modifications, or drug discontinuations. Significant and prolonged changes in host gene expression were observed at Day 84.6,29 Extended follow up for 24 months demonstrated that vorinostat did not cause any long-term safety issues or changes in HIV expression.30
RIVER trial (NCT02336074)
In this Phase 2 study, 97% (29/30) of participants in the intervention arm (ART plus two therapeutic HIV vaccines plus vorinostat) experienced an AE. Seventy percent of these AEs were mild and 23% were moderate in intensity. In comparison, in the ART-only arm, 73% (22/30) of participants experienced an AE, 33% of which were mild and 20% of which were moderate. No intervention-related SAEs were reported.17,18,31
A substudy evaluating the CNS impacts of trial interventions found no evidence of increased neuronal damage with ART, therapeutic vaccination, and vorinostat compared to ART alone.32
MOXIE trial (NCT03382834)
In this Phase 2 study, 21 women were assigned to receive vorinostat plus tamoxifen and 10 women were assigned to receive vorinostat alone. No Grade 3 or higher drug-related AEs were reported during the study.20,21
Additional AEs known to be associated with vorinostat use are described in the FDA-approved Full Prescribing Information for Zolinza.4
Drug Interactions
Previous studies have indicated that vorinostat at the 400-mg dose level does not inhibit CYP-drug-metabolizing enzymes. Because vorinostat is not eliminated via CYP pathways, drug-drug interactions between vorinostat and agents that are known CYP inhibitors or inducers are not anticipated. Vorinostat is not a substrate of human P-gp and is not likely to inhibit P-gp at a serum concentration of 2 µM (maximum plasma concentration [Cmax]) in humans.4
During a Phase 2 study (NCT01365065), which involved 20 participants who received at least three ARV agents and once-daily vorinostat over 14 days, there were no significant interactions between vorinostat and ART.6
Additional known interactions between vorinostat and coadministered drugs are described in the FDA-approved Full Prescribing Information for Zolinza.4
References
- National Center for Biotechnology Information. PubChem Compound Summary for CID 5311, vorinostat. Accessed January 6, 2026
- Treatment Action Group website. Research toward a cure trials. Accessed January 6, 2026
- Rasmussen TA, Tolstrup M, Winckelmann A, Østergaard L, Søgaard OS. Eliminating the latent HIV reservoir by reactivation strategies. Hum Vaccines Immunother. 2013;9(4):790-799. Accessed January 6, 2026
- Merck Sharp & Dohme Corp. Zolinza: full prescribing information, November 2024. DailyMed. Accessed January 6, 2026
- Matalon S, Rasmussen TA, Dinarello CA. Histone deacetylase inhibitors for purging HIV-1 from the latent reservoir. Mol Med. 2011;17(5-6):466-472. Accessed January 6, 2026
- Elliott JH, Wightman F, Solomon A, et al. Activation of HIV transcription with short-course vorinostat in HIV-infected patients on suppressive antiretroviral therapy. PLoS Pathog. 2014;13(10(11)):e1004473. doi: 10.1371/journal.ppat.1004473. Accessed January 6, 2026
- Bartholomeeusen K, Fujinaga K, Xiang Y, Peterlin BM. Histone deacetylase inhibitors (HDACis) that release the positive transcription elongation factor b (P-TEFb) from its inhibitory complex also activate HIV transcription. J Biol Chem. 2013;288(20):14400-14407. doi:10.1074/jbc.M113.464834. Accessed January 6, 2026
- Shirakawa K, Chavez L, Hakre S, Calvanese V, Verdin E. Reactivation of latent HIV by histone deacetylase inhibitors. Trends Microbiol. 2013;21(6):277-285. doi:10.1016/j.tim.2013.02.005. Accessed January 6, 2026
- University of North Carolina, Chapel Hill. A Phase I/II investigation of the effect of vorinostat (VOR) on HIV RNA expression in the resting CD4+ T cells of HIV-infected patients receiving stable antiretroviral therapy. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on March 17, 2011. NLM Identifier: NCT01319383. Accessed January 6, 2026
- Archin NM, Kirchherr JL, Sung JAM, et al. Interval dosing with the HDAC inhibitor vorinostat effectively reverses HIV latency. J Clin Invest. 127(8):3126-3135. doi:10.1172/JCI92684. Accessed January 6, 2026
- Archin NM, Liberty AL, Kashuba AD, et al. Administration of vorinostat disrupts HIV-1 latency in patients on antiretroviral therapy. Nature. 2012;487(7408):482-485. doi:10.1038/nature11286. Accessed January 6, 2026
- Archin NM, Bateson R, Tripathy M, et al. HIV-1 expression within resting CD4+ T cells after multiple doses of vorinostat. J Infect Dis. 2014;210(5):728-735. doi:10.1093/infdis/jiu155. Accessed January 6, 2026
- SEARCH Research Foundation. A randomized study to compare the efficacy of vorinostat/hydroxychloroquine/maraviroc (VHM) in controlling HIV after treatment interruption in subjects who initiated ART during acute HIV infection. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on June 3, 2015. NLM Identifier: NCT02475915. Accessed January 6, 2026
- SEARCH Research Foundation. Study SEARCH 026 Assessment of the HIV CNS reservoir, neurological and neuro-cognitive effects, and source of rebound HIV in CNS in subjects participating in Study SEARCH 019. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on June 2, 2015. NLM Identifier: NCT02470351. Accessed January 6, 2026
- Kroon EDMB, Ananworanich J, Pagliuzza A, et al. A randomized trial of vorinostat with treatment interruption after initiating antiretroviral therapy during acute HIV-1 infection. J Virus Erad. 2020;6(3):100004. doi:10.1016/j.jve.2020.100004. Accessed January 6, 2026
- Bayside Health. A pilot study to assess the safety and effect on HIV transcription of vorinostat in patients receiving suppressive combination anti-retroviral therapy. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on June 1, 2011. NLM Identifier: NCT01365065. Accessed January 6, 2026
- Imperial College London. Research in viral eradication of HIV reservoirs. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on October 23, 2014. NLM Identifier: NCT02336074. Accessed January 6, 2026
- Fidler S. RIVER research in viral eradication of HIV reservoirs: a two-arm (proof of concept) randomised Phase II trial vorinostat plus a prime boost vaccine. Slides presented at: International AIDS Conference (AIDS 2018): July 23-27, 2018; Amsterdam, the Netherlands. Accessed January 6, 2026
- Fidler S, Stöhr W, Pace M, et al. Antiretroviral therapy alone versus antiretroviral therapy with a kick and kill approach, on measures of the HIV reservoir in participants with recent HIV infection (the RIVER trial): a phase 2, randomised trial. Lancet Lond Engl. 2020;395(10227):888-898. doi:10.1016/S0140-6736(19)32990-3. Accessed January 6, 2026
- National Institute of Allergy and Infectious Diseases (NIAID). Selective estrogen receptor modulators to enhance the efficacy of viral reactivation with histone deacetylase inhibitors. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on December 19, 2017. NLM Identifier: NCT03382834. Accessed January 6, 2026
- Scully E, Tsibris A, Aga E, et al. Effect of tamoxifen on vorinostat-induced HIV RNA expression in women on ART (ACTG A5366): the MOXIE trial. Poster presented at: Conference on Retroviruses and Opportunistic Infections (CROI); March 8-11, 2020; Boston, MA. Poster 333. Accessed January 6, 2026
- Scully EP, Aga E, Tsibris A, et al. Impact of tamoxifen on vorinostat-induced HIV expression in women on antiretroviral therapy (ACTG A5366:The MOXIE trial). Clin Infect Dis. Published online February 17, 2022:ciac136. doi:10.1093/cid/ciac136. Accessed January 6, 2026
- University of North Carolina, Chapel Hill. IGHID 11627 - A Phase I study to evaluate the effects of vorinostat and HIV-1 antigen expanded specific T cell therapy (HXTC) on persistent HIV-1 infection in HIV-infected individuals started on antiretroviral therapy (The XTRA Study). In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on July 11, 2018. NLM Identifier: NCT03212989. Accessed January 6, 2026
- University of North Carolina, Chapel Hill. IGHID 11802 - Combination Therapy With the Novel Clearance Modality (VRC07-523LS) and the Latency Reversal Agent (Vorinostat) to Reduce the Frequency of Latent, Resting CD4+ T Cell Infection (The VOR-07 Study). In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on: January 10, 2019. NLM Identifier: NCT03803605. Accessed January 6, 2026
- University of North Carolina, Chapel Hill. IGHID 12430 - Deliver-02 - A Phase 1, open label, randomized study to evaluate the safety and tolerability of MGD014 and MGD020 with a latency reversal agent versus temporary treatment interruption in persons with HIV-1 on antiretroviral therapy. In: ClinicalTrials.gov. Bethesda (MD): National Library of Medicine (US). Registered on: October 13, 2025. NLM Identifier: NCT07217379. Accessed January 6, 2026
- Robertson K, Kuruc J, Gay C, Archin N, Eron J, Margolis D. Preliminary assessment of the neurocognitive effects of vorinostat administration in HIV eradication. Abstract presented at: International AIDS Conference; July 20-25, 2014; Melbourne, Australia. Abstract WEPE018. Accessed January 6, 2026
- Kroon E, Ananworanich J, Eubanks K, et al. Effect of vorinostat, hydroxychloroquine and maraviroc combination therapy on viremia following treatment interruption in individuals treated during acute HIV infection. 21st International AIDS Conference (AIDS 2016); July 18-22, 2016; Durban, South Africa. Mascolini: Vorinostat, HCQ, Maraviroc Do Not Delay Time to Rebound After Interruption. Conference reports for National AIDS Treatment Advocacy Project (NATAP); 2016. Accessed January 6, 2026
- Kroon E, Ananworanich J, Le LT, et al. Central nervous system impact of vorinostat, hydroxychloroquine and maraviroc combination therapy followed by treatment interruption in individuals treated during acute HIV infection (SEARCH 026). International AIDS Conference; July 18-22, 2016; Durban, South Africa. Levin: Conference reports for National AIDS Treatment Advocacy Project (NATAP); 2016. Accessed January 6, 2026
- Elliott J, Solomon A, Wightman F, et al. The safety and effect of multiple doses of vorinostat on HIV transcription in HIV-infected patients receiving combination antiretroviral therapy. Abstract presented at: Conference on Retroviruses and Opportunistic Infections (CROI); March 3-6, 2013; Atlanta, GA. Abstract 50LB. Accessed January 6, 2026
- Mota TM, Rasmussen TA, Rhodes A, et al. No adverse safety or virological changes 2 years following vorinostat in HIV-infected individuals on antiretroviral therapy. AIDS. 2017;31(8):1137-1141. doi:10.1097/QAD.0000000000001442. Accessed January 6, 2026
- Fidler S, Stohr W, Pace M, et al. A randomised controlled trial comparing the impact of antiretroviral therapy (ART) with a “Kick-and-Kill” approach to ART alone on HIV reservoirs in individuals with primary HIV infection (PHI); RIVER trial. Abstract presented at: International AIDS Conference (AIDS 2018); July 23-27, 2018; Amsterdam, the Netherlands. Abstract TUAA0202LB. Accessed January 6, 2026
- Alagaratnam J, Stöhr W, Toombs J, et al. No evidence of neuronal damage as measured by neurofilament light chain in a HIV cure study utilising a kick-and-kill approach. J Virus Erad. 2021;7(3):100056. doi:10.1016/j.jve.2021.100056. Accessed January 6, 2026
Last Reviewed: January 6, 2026